Posted on: May 7, 2021
By Franciscah Nzanga (1), Tabitha Mberi (1), Stephen Odindo (1), Isaac Mwangi (1), Beatrice Wasunna (2) and Michael Onsando (3)
Illustration by Anthony Mogaka

In Joseph Heller’s military novel Catch-22, a pilot could never be deemed insane unless he requested an evaluation. If a pilot requested for an evaluation, then he would be deemed sane as the act of requesting evaluation would be one of a sane man. The pilots were trapped in a loop of rules – the catch. COVID-19 left us in a similar situation with healthcare infrastructure. On one hand, we were looking to avoid crowded areas while on the other we needed to be tested and cared for. Many people found themselves afraid to go for COVID tests and other facility-based services, lest they catch the illness while waiting in line. Nearly overnight, digital healthcare was infused into the clinical workday as patients and providers alike were forced to become fast adopters.
However, digital healthcare is not the only care patients need. While digital healthcare delivered tools and technologies, virtual healthcare provides patients with the support needed for wellness, diagnosis and treatment regardless of their location. Digital healthcare may have accelerated but we found the themes of the Accenture 2020 digital health consumer research still ring true: consumers are interested in virtual services, but a cumbersome digital experience turns them off. They are concerned over whether they can trust the services, over their privacy and security. Clinicians are struggling with integrating new tools and services into their day-to-day clinical workflows.
The Community Health Innovation Network (CHIN) is a three-year program initiative by Living Goods and Medic. The network promotes creative solutions by designing and testing a pipeline of innovative ideas that integrate community health care with health facilities while extending high-quality diagnostic technologies to effectively reach clients at the community level. It features a Virtual Design Lab or vLab composed of a small team with members from Living Goods, Medic, Accenture Development Partnerships, and the Busara Center for Behavioral Economics. As the vLab, our objective is to ensure three things:
- The CHIN benefits from community engagement
- A human-centred approach is used in the design of all health interventions, despite the travel restrictions necessitated by the COVID-19 pandemic.
- Monitoring and evaluation of current programs continue via remote means
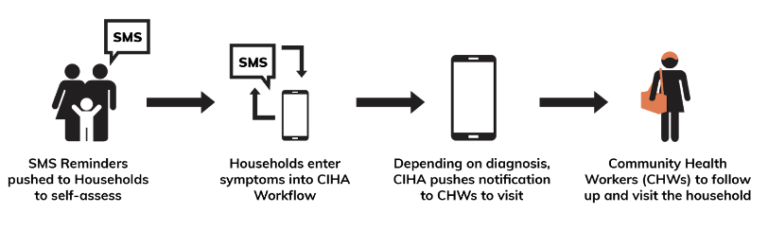
We run experiments using a self-triage platform that allows users to assess themselves by indicating their symptoms on an SMS workflow. The platform then analyses their responses and predicts the likelihood of a certain illness outcome. It aims to empower caregivers and household members, allowing them to screen themselves and initiate access to healthcare.
While the user experience assessments indicated that the platform was of great value to the community; various barriers such as lack of digital literacy, infrastructure, shared mobile phones and trust hampered rapid adoption. These barriers indicate a need for virtual health solutions built on values that include trust, transparency and accountability; designed to meet the African context.
Education levels also seem to affect the amount of time taken to complete SMS service-experience workflows: clients with a post-secondary school level education completed the workflows more than twice as fast (7 minutes) as those without (15 minutes). This validates the hypothesis that a lack of literacy is a hindrance to recent digital and virtual health gains.
While the healthcare industry prioritized one type of convenient care, consumer
expectations raced ahead—and those expectations are largely unmet. Approximately 70 per cent of all consumers are interested in receiving a range of health and care services virtually, yet only 20 per cent have experienced virtual healthcare. Virtual care offers what consumers really want: a variety of health and care services available to any location at any time, from health and wellness to episodic injury and illness to ongoing condition management. It brings a wide range of healthcare services to consumers, independent of physical location.
In addition, virtual makes it easier for people to be actively involved in their own health and care. Unlike in-person care, virtual care can scale affordably.
Some simple behavioral nudges are proving effective towards improving uptake such as:
- Day & Time of Engagement – data showed that clients are more responsive and willing to complete an assessment in the afternoon and towards the end of the week or on weekends.
- Message Language – clients responded better to messages written in Swahili but generally, there was no statistically significant difference in the completion rate between the two languages
- Message Structure – A clear call to action in a message gives a better response and completion rate
- Use of support marketing tools – Distribution of behavior change communication materials such as stickers and flyers with the virtual care phone number. This can be stuck on the wall or door of the homesteads and used as needed.
- Community Health Worker motivation through the provision of financial and non-financial incentives. This motivates them to act as champions for the platform.
Consumers want the best of both in-person and virtual care and the ability to select and switch from one type to the other whenever they want – and it is this that the healthcare system must strive to give them. Here are some actions that can help your organisation initiate or accelerate virtual services that your customer needs:
- Pursue quick wins to protect against disruption – Services like eVisits – asynchronous secure message-based encounters between patient and physicians – can be executed simply and relatively quickly. Other first-phase options can be virtual mental health services and automated reminders (for appointments, medications and more) to support care plan compliance. At the same time, workflow redesign and change management will be needed to help clinicians adapt to and adopt these new virtual models.
- Support consumer models of health: As self-triage and self-care becomes the norm, traditional health care providers – both government-led and private – will undergo significant pressure to accommodate a consumer model of healthcare in low and middle income countries. To support these changed power relationships and roles, providers will need new tools to manage self-triage workflows. One concept is the virtual helpdesk, a tablet-based environment that allows the provider such as the facility nurse-in-charge or chief medical officer to manage multi-channel workflow requests and assist the triage of cases. Some cases will be automatically routed to an appointment scheduler, others will be referred to a CHW for call-out service. Urgent workflows may connect the provider directly to the client via Whatsapp in real-time, effectively telemedicine for low-resource settings. The provider becomes the facilitator of care rather than gatekeeper.
- Explore a full portfolio of choices that appeal to the next – generation consumer – With foundational services in place, organizations can move to establish a full range of community healthcare services including telemedicine services, remote monitoring of those with chronic conditions, post-discharge follow up and even in-home therapies. These services should be accessible to consumers who are healthy, temporarily ill and injured, or those with ongoing health issues. It is worth noting that creating this portfolio will require collaboration with key stakeholders and users, as well as testing to ensure the services will be used optimally.
- Reimagine and reinvent the community healthcare model – Virtual approaches enable family, friends and other non-clinical caregivers to be part of clinical encounters. It’s time to move away from the traditional model of care that assumes that clinicians are the only caregivers. Half of the consumers surveyed say a family member is involved with their health and healthcare.
At the vLab, we are proving that a working self-assessment flow can be configured and deployed successfully and quickly. The user journey is functioning, with clients able to indicate symptoms, self-triage and receives follow-ups from the CHW.
Integrated health services that combine virtual and physical care are the key to re-inventing health and care services for Africa – and the time to do it is now.
(1) Living Goods
(2) Medic
(3) Busara Center for Behavioral Economics
. . .
Connect with us on our social media platforms: Twitter, Facebook, Instagram, & LinkedIn.
